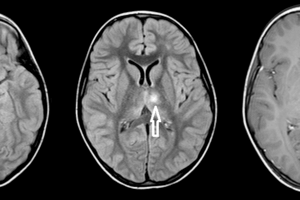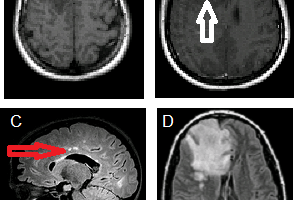
Sarcoidosis is a systemic inflammatory condition with a specific pathology – non caseating (unlike TB) granulomas. The condition affects the lungs , bones and brain. Neurosarcoid occurs in about 5-10% of patients with sarcoidosis and is often asymptomatic, although may present with a myriad of neuropsychiatric symptoms, ranging from facial nerve palsy to depression.
Leptomeningeal (pial and arachnoid) involvement with perimedullary enhancement is most common, with preferential involvement of the parasellar region and the cranial nerves, especially the optic chiasm. Predilection for these spaces can help distinguish sarcoid from other causes of leptomeningeal enhancement like meningitis, metastatic disease, vasculitis and subacute infarct. Enhancing intraparenchymal granulomas may also be seen in neurosarcoid. Complications include hydrocephalus and vasculitis.
Diagnosis: Neurosarcoid

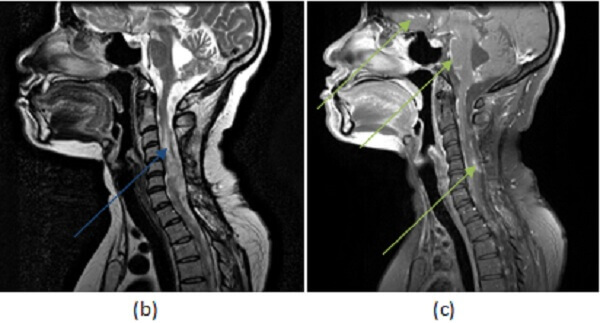
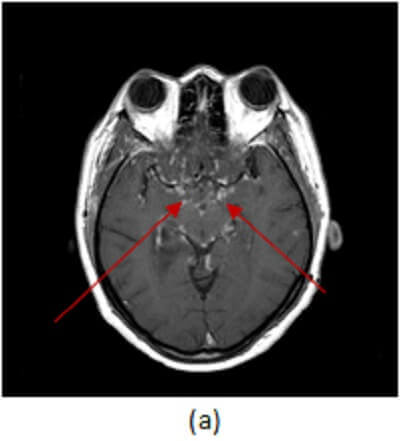
Figure 1: (a, red arrow) axial postcontrast T1 demonstrates enhancement of the leptomeningeal surface along the basal cisterns. (b, blue arrow) Sagittal T2 of the spine demonstrates increased T2 signal involving an expanded cervical cord. (c, green arrow) Sagittal T1 post contrast of the spine and brain demonstrates intramedullary and leptomeningeal enhancement of the cervical cord, along with parasellar, frontal and cerebellar leptomeningeal enhancement.
The cord is involved in about 25% of neurosarcoid cases – leptomeningeal and intraparenchymal enhancement are the most common findings. There is no disease modifying therapy for sarcoidosis yet available. Corticosteroids are helpful in reducing the extent of inflammation.